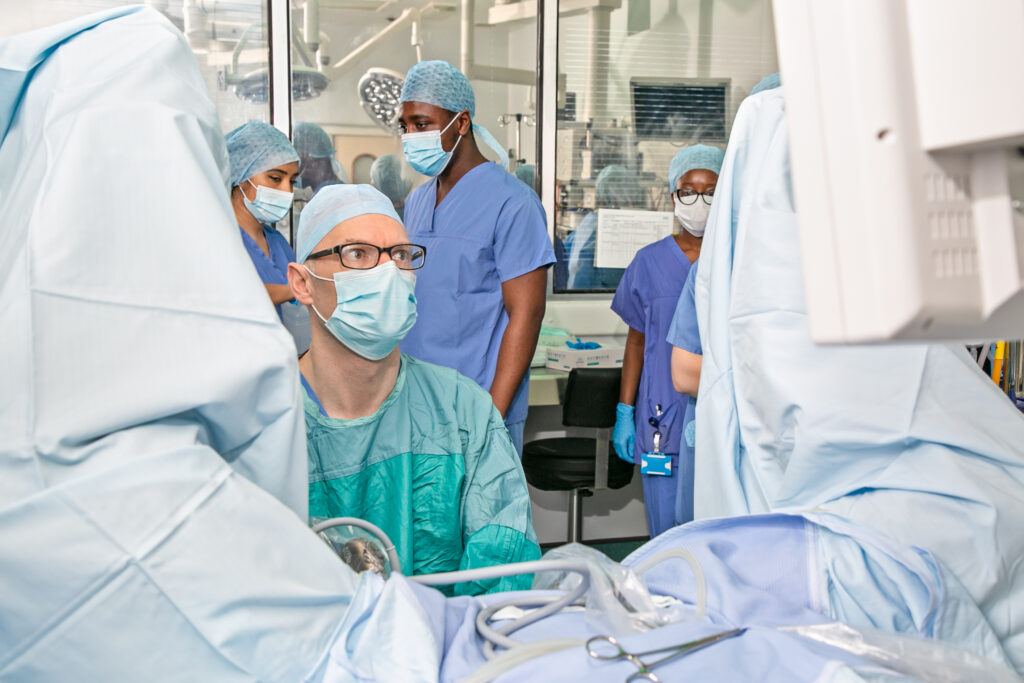
A SURGICAL team from Bradford Teaching Hospitals NHS Foundation Trust has played a key role in a pioneering trial which could help improve quality-of-life for patients with rectal cancer.
Surgery can often cure early-stage rectal cancer. But in the standard operation, the surgeon will remove the whole rectum, significantly impacting a patient’s quality-of-life, and often leaving patients with a permanent stoma or colostomy.
Consultant colo-rectal surgeons Mark Steward and Jon Robinson have favoured a less-invasive approach for patients with early rectal cancer, and have been treating some of the Trust’s patients in this way since 2006 using a technique called TEMS (trans-anal endoscopic microsurgery).
TEMS, by contrast to major surgery, is carried out using a specially designed microscope and instruments, allowing it to be performed through the anus (back passage) inside the rectum, requiring no incisions on the outside of the anus or abdomen, and preventing patients requiring lifelong stomas.
Through their development and expertise in TEMS surgery, Mr Steward and Mr Robinson along with their clinical team at Bradford Royal Infirmary have been major contributors to the TREC (Trans-anal Microscopic Surgery for Early Rectal Cancer) study.
The TREC trial assessed whether radiotherapy followed by surgery to remove the part of the rectum affected by cancer using TEMS worked better than surgery to remove the whole rectum.
Significant improvement
The study’s results – recently highlighted in The Lancet – are encouraging as for the first time they demonstrated evidence of significant improvement in quality-of-life among the organ preservation group and fewer side effects.
“TEMS was originally used for removing polyps from the rectum and some early cancer where the patient was perhaps too old or too frail to tolerate regular treatment,” said Mr Steward.
“But we have been dealing with rectal cancer using a combination of radiotherapy and TEMS since 2006, and have treated more than 150 patients this way since then.
“The author of the TREC study, Simon Bach from the University of Birmingham, wanted to recruit people into a trial to compare the use of radiotherapy combined with TEMS to treat rectal cancer. And we were one of the main contributors in the UK.
“The results have now demonstrated that you can adopt this technology in the treatment of early-stage rectal cancer and provide a better quality-of-life, and that you can adopt it without compromising outcomes, which have been favourably comparable.
“Traditional treatment can have higher risks which affect quality-of-life.
“Combining radiotherapy and TEMS treatment is shorter, less painful and less likely to result in the need for a stoma (colostomy bag).
“The results have now generated a second study called STAR-TREC, which is looking in more detail at the use of this technique.”
New approach
Mr Steward said that around a quarter of the 11,500 rectal cancers diagnosed in the UK each year could benefit from the new approach.
“The combination of radiotherapy and organ preserving surgery has benefited many with breast, and head and neck cancers, for example, but until very recently management of rectal cancer had lagged behind.
“But we now have patients who have a better quality-of-life because of the treatment they received at Bradford.
“And with the increase of bowel screening programmes nationwide which will pick up more cases of early-stage rectal cancer, it makes sense to explore more acceptable treatments nationally.”
Further testing and analysis is now needed to see whether the TEMS approach should be adopted throughout the country.
Mr Steward added that the Bradford Teaching Hospitals team had continued to treat patients with rectal and colon cancer throughout the pandemic.
Mr Steward and Mr Robinson have also recently completed a 12-year experience of their work using TEMs to treat rectal cancer, which is due to be published in the International Journal of Colorectal Diseases.
Picture caption: Mr Robinson and members of the surgery team at work
ENDS
For further media information, please contact communications@bthft.nhs.uk