Thyroid cancer
This video is for patients who have been diagnosed with thyroid cancer. It explains the care pathway, including surgery and treatment options, what to expect during recovery, and how to get support.
Please watch the video and also read through the information on this page. Useful links and contact details are provided so you know where to go for more help.
Meet the team

Mohammad Adeel
ENT Consultant

Sarah Hillary
Cancer Nurse Specialist
Contact us
- Thyroid Cancer Specialist Nurse: 01274 365848 Monday to Friday, 8am to 5pm excluding bank holidays. Outside of these times please leave a message and we will call back as soon as possible.
- Ward contact details: provided when you leave hospital. Ask staff before discharge if you do not have them.
About thyroid cancer
Diagnosis
If your GP suspects thyroid cancer, you will be referred to a hospital specialist.
You may have:
- an examination of your neck and vocal cords
- an ultrasound scan of the thyroid – During this if the specialist feels there is an area of concern they will take a fine needle aspiration (FNA) or Core biopsy to collect cells or tissue for testing.
Sometimes this can not provide all the information we need to give a diagnosis. If this is the case a diagnostic hemithyroidectomy would be recommended.
Sometimes it is not possible to confirm if something is a cancer from ultrasound and fine needle aspiration. In these cases, a diagnostic lobectomy may be recommended
If cancer is confirmed, your case will be discussed at a regional multidisciplinary team meeting (MDT). This is a group of specialists who agree the best treatment plan for you. Following this meeting your specialist will explain the outcome and recommendations.
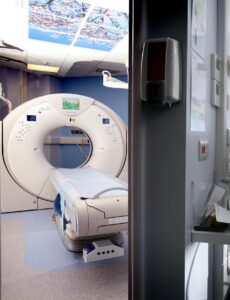
You may also need scans such as CT or MRI.
You will also be offered a holistic needs assessment by telephone to check your wider needs and provide support.
Treatment
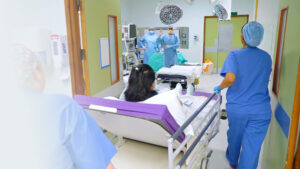
Surgery
You may need one or more of the following:
- Hemithyroidectomy: removal of one lobe of the thyroid.
- Total thyroidectomy: removal of the whole thyroid gland.
- Neck dissection: removal of lymph nodes in the neck.
Your surgeon will explain which operation is recommended for you, why it is needed, and any risks. You will also be given written information.
Most people stay in hospital for one night and go home the day after surgery. You may have:
- a neck drain, removed before discharge
- stitches that either dissolve on their own or are removed later by your GP practice
You will get a phone call around two weeks after surgery to check on your recovery and explain next steps.
Levothyroxine
The thyroid makes a hormone called thyroxine. If all of your thyroid is removed, you will need to take levothyroxine tablets for life.
Sometimes, even if only half the thyroid is removed, you may still need levothyroxine. This will be decided by how you feel and through blood tests.
Radioactive Iodine (RAI)
Some patients are advised to have radioactive iodine treatment after surgery. This is given in Leeds by the oncology team.
- It is usually given as a capsule.
- You will stay in an isolation room for a few days.
- You may need to follow safety advice at home for 1–2 weeks.
Before treatment, you will meet the oncology team to discuss why it is recommended and what to expect. You may also need to follow a low-iodine diet and have hospital injections beforehand.
You will meet the specialist nurses at Leeds and they will be your contact during this treatment.
After Treatment
Results
Anything removed during surgery is sent to the laboratory (histopathology). Results usually take a few weeks. Once available, your surgeon will meet with you to explain what they mean and whether more treatment is needed.
Follow-up and Support
You will see your surgeon a few weeks after surgery. Longer-term follow-up usually includes:
- ultrasound scans
- blood tests
Depending on your treatment, you will be seen by either the ENT team or the Endocrinology team.